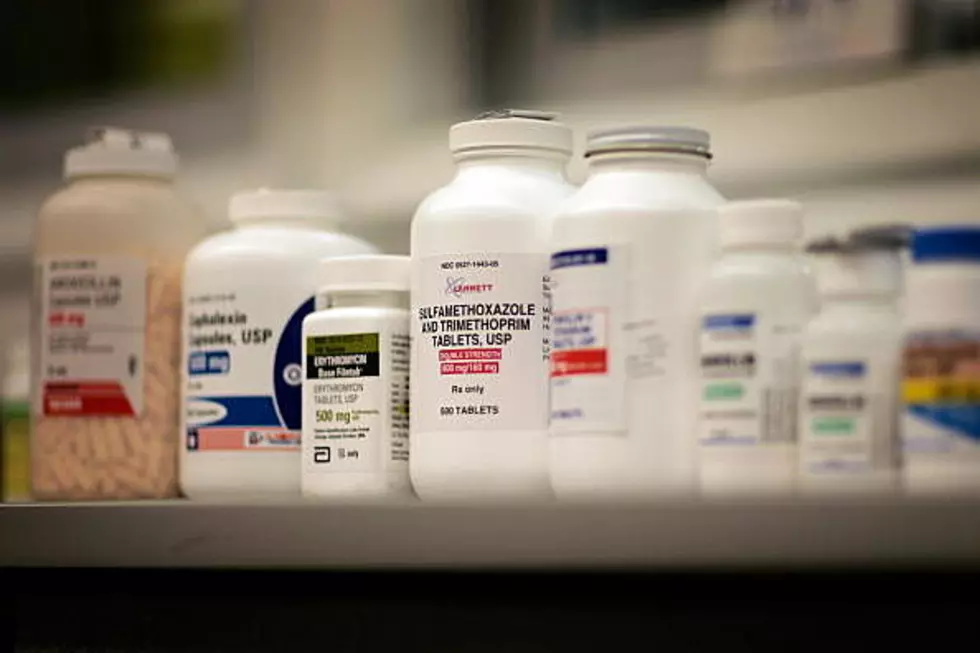
Pharmacy Case Settled – Prescription Drug Saving Initiative
Prime Therapeutics, the pharmacy benefit manager of Blue Cross and Blue Shield of Montana, has settled a case with State Insurance Commissioner Matt Rosendale’s office and agreed to pay up to $375,000 for an independent examination of its data.
Spokesman Kyle Schmauch explains.
“Prime Therapeutics is the middle man that manages a lot of the prescription drug transactions for Blue Cross Blue Shield of Montana,” said Schmauch. “As part of a settlement against them, they have agreed to pay up to $375,000 to have their data analyzed by a third party firm.”
Schmauch said ever since Matt Rosendale became State Auditor and Insurance Commissioner, he has been working to find ways to bring down the high cost of prescription drugs.
“The Drug Savings Initiative, as we call it, has included legal actions against pharmaceutical industry middle men such as Prime Therapeutics,” he said. “As part of our investigation, we found that they were out of compliance with some of Montana’s insurance laws and the settlement this week is part of that legal action. Their data will help us dive deeper into the reason why prescription drugs costs are so high.”
Schmauch said the middle men such as Prime Therapeutics force prescription costs higher and higher.
“Things we consider to be price gouging, where they are charging the insurance company far more for a drug than they reimburse to a pharmacy,” he said. “Claw backs, where they will come and take money back out of the hands of the pharmacy after a transaction has been completed and kickbacks between these pharmacy benefit managers and drug manufacturers that only serve to drive up the price of drugs and do nothing to help the patient afford the prescription medications they need.”
Click here for a new webpage that outlines the Rosendale Drug Savings Initiative for the public and includes links to relevant legislation, presentations, and news reports.
More From KMMS-KPRK 1450 AM






![The Bozeman Warming Center Needs Your Help [Listen]](http://townsquare.media/site/8/files/2018/12/GettyImages-925423514.jpg?w=980&q=75)

